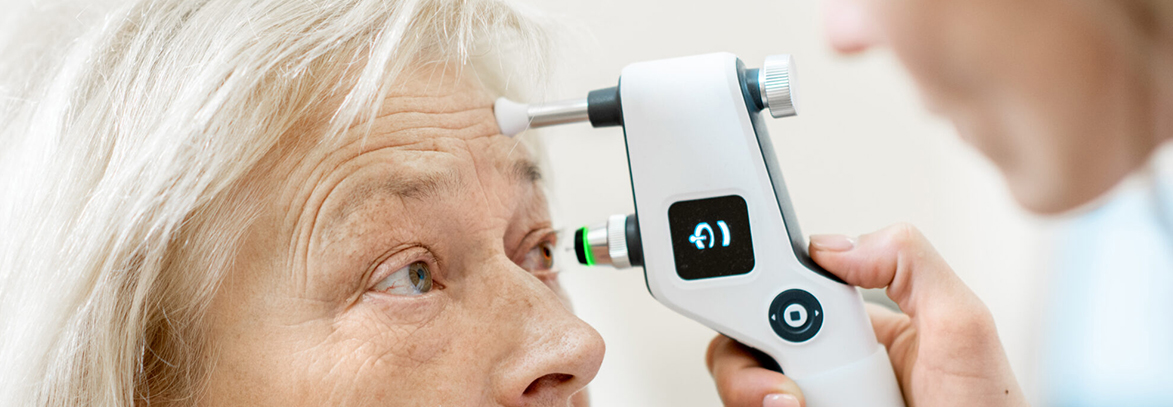
What is glaucoma (high eye pressure)?
Glaucoma, or high eye pressure, is an insidious disease characterized by intraocular pressure that is usually higher than it should be, resulting in long-term damage to the optic nerve and permanent vision loss. Often asymptomatic, it can be diagnosed during routine examinations by measuring intraocular pressure and examining the fundus and optic nerve. Risk factors for glaucoma include advanced age, a family history of glaucoma, pseudoexfoliation, previous intraocular surgery, long-term use of steroid eye drops, nasal sprays, or systemic treatments, and a history of eye trauma.
Glaucoma is generally seen in middle-aged and older individuals, but it can also occur in children and infants.
Glaucomas are basically divided into two types: open-angle and closed-angle glaucoma. Most patients have open-angle glaucoma. As mentioned earlier, this type has no symptoms, while in closed-angle glaucoma, eye and headaches may occur from time to time. Sometimes, severe eye and headaches, eye redness, and decreased vision can occur, leading to an angle-closure crisis that requires emergency treatment.
In congenital glaucoma, the baby’s eye may enlarge and the transparent part of the eye may become cloudy.
How should glaucoma be diagnosed and monitored?
In patients suspected of or diagnosed with glaucoma, intraocular pressure, optic nerve examination, visual field testing, and regular monitoring of these parameters are crucial. To detect progression, optical coherence tomography and visual field tests should be performed regularly at specific intervals.
Optical coherence tomography (OCT) detects structural losses that occur in the early stages, while visual field testing detects functional losses that occur in later stages. Both tests are crucial for diagnosis and treatment monitoring.
Why are early diagnosis and treatment of glaucoma important?
Glaucoma (high eye pressure) progresses without symptoms and, if diagnosed late and left untreated, can result in permanent blindness. This can only be prevented with early diagnosis and treatment. Regular eye checkups and intraocular pressure (IOP) measurements are important for early diagnosis.
When should intraocular pressure (IOP) be measured in healthy individuals?
After the age of 40, IOP measurements should be taken annually.
Risk factors;
- If there is a family history of glaucoma
- High myopia
- If you are receiving cortisone treatment
- If you have suffered trauma to your eye or head
- Regular eye examinations are necessary in the presence of certain co-existing eye conditions (such as pseudoexfoliation (cottonychia-like or flaky texture), uveitis, Sturge-Weber syndrome (port-wine stain), and a history of intraocular surgery) as risk factors.
After age 40, more frequent check-ups may be necessary if these risk factors are present.
Regular eye pressure measurements should be taken before the age of 40 if these risk factors are present.
What is the normal value for intraocular pressure?
Intraocular pressure (IOP) in the population shows a curve that follows a normal distribution and slopes to the right. The average IOP in adults is 15±3.0 mmHg. The upper limit of normal IOP is defined as two standard deviations above this average value, i.e., 21 mmHg, and IOP above this level is considered high. However, normal or glaucoma diagnosis cannot be made solely based on IOP measurement. Higher IOP is a significant risk factor for both the development and progression of glaucoma. However, in some cases, glaucoma does not occur when IOP is above 21 mmHg, while in other cases, it can cause damage to the optic nerve even when it is below 21 mmHg. Therefore, IOP measurement alone is not sufficient to diagnose glaucoma (high eye pressure).
What tests are recommended for the initial assessment during an eye pressure examination ?
Visual acuity and refractive error.
Biomicroscopic (slit lamp) examination
Gonioscopy (angle) examination
Eye pressure measurement (with an applanation (blue light) tonometer, and in infants and children with handheld devices such as i-care or Tonopen)
Visual field (VF) test
Fundus examination and Optical Coherence Tomography (OCT) for clinical evaluation of the optic nerve head (ONH), retinal nerve fiber layer (RNFL), and macula (ganglionic cell complex analysis).
Central corneal thickness (CCT)
Depending on the patient’s age and eye condition, these tests may include ultrasonography, ultrasound biomicroscopy (UBM), axial length measurement, and white-to-white (WTW) measurement.
* The page content is for informational purposes only. This information has been prepared in accordance with the “Regulation on Promotion and Information Activities in Health Services” published in the Official Gazette dated 12.11.2025. Results may vary from person to person in every surgical or interventional procedure. For diagnosis and treatment, please consult your doctor.
Glaucoma (Eye Pressure)
Neque porro est qui dolorem ipsum quia quaed inventore veritatis et quasi architecto beatae vitae dicta sunt explicabo. Aelltes port lacus quis enim var sed efficitur turpis gilla sed sit amet finibus eros. Lorem Ipsum is simply dummy text of the printing and typesetting industry.


